Training Materials for Injecting Drug Users and their Social Network

- This training course is optional and should be applied with the WINGS of Hope participants who feel overdose applies to their situation.
- This module has been developed by Dr Timothy Hunt at Columbia University Social Intervention Group, and builds on guidelines and materials designed as a part of Project ADVANCE by Attika Foundation and Kyrgyz Harm Reduction Association team led by Sergei Bessonov whose efforts we very much appreciate.

- Discuss with participant overdose in Kyrgyzstan.
- While discussing, use and refer to overdose statistics collected as a part of the WINGS of Hope project.
- Before discussing overdose in details, let’s talk briefly about overdose in Kyrgyzstan. It is difficult to estimate the true number of overdose patients and the number of fatal overdoses in Kyrgyzstan, but overdose is the leading cause of death among people who inject drugs in Kyrgyzstan and many other countries. Experiencing overdose “ever” was reported by 46% of the participants, and 6% overdosed in the past 3 months. About 32% of project participants stated that they were able access Naloxone through NGOs. In the framework of study, the respondents (n=213) also shared that they knew approximately 465 people who experienced overdose in the past 3 months. According to the participants’ estimates, out of 465, at least 208 persons (44,7%) died from overdoses.
- One of the biggest problems with treatment of overdose patients in Kyrgyzstan is the lack of appropriate medical facilities and qualified toxicologists. Often, people are embarrassed or fearful about seeking help, as well.
- Drug treatment in Kyrgyzstan remains hard to access for injection drug users and is even less accessible to women who use drugs because of public stigma, which discourages them from seeking help. Actually, treatment is limited mainly to paid and costly detox programs. Methadone service is available and free, but requires being officially registered in medical records as drug user. This requirement scares people and discourages them from joining methadone therapy as they are uncertain about negative consequences of this registration in a longer run. A total of number of women who use drugs enrolled in methadone program is 94. It is approximately 20.8% of the number of registered WDU or 4.8% of the estimated number.
- Therefore, it is important for us to learn skills how to minimize the risk of an overdose and know what to do if a friend or a partner is overdosing. There are medications that can help in the immediate response to an overdose while getting emergency help. We will be introducing you to an option called Naloxone and how you can obtain it as part of this project.

- Briefly review what and how opiates work.
- Provide examples of opiates.
- Describe the effects of opiates on brain and central nervous system.
- Opiates are a type of drug that comes from the opium poppy or are synthetically made by a drug company. All opiates act the same way on the brain. Opiates are depressants, which mean they slow down your central nervous system, including breathing.
- Can you think of an example of an opiate? Examples of natural opiates include heroin, morphine and codeine. Examples of synthetic (or manufactured) opiates include methadone, oxycontin, percodan, percocet, and vicodin.
- Opiates differ in both their strength and in the length of time they act on your body. For example, heroin is a strong opiate that produces effects for 6-8 hours. Methadone is a strong opiate, too, but acts much longer in your body – between 24 and 32 hours. Codeine is a weak opiate whose effects last for 3-4 hours:
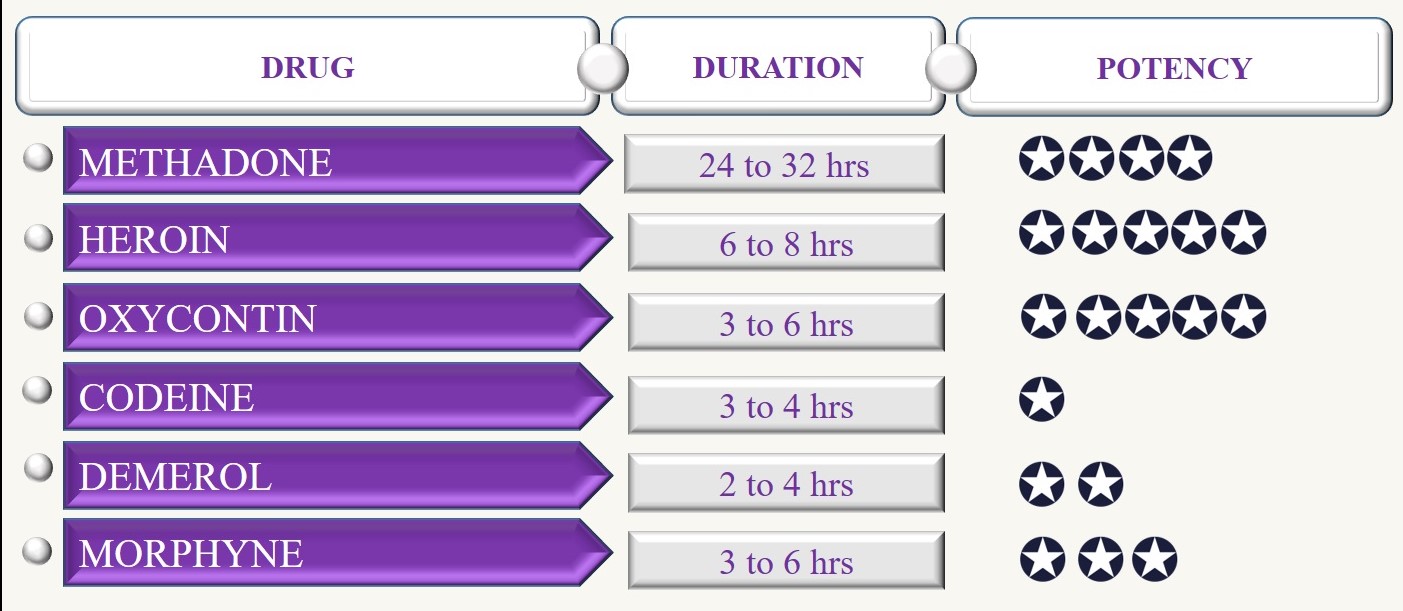
?

- Discuss causes of an opiate overdose.
- Provide examples to better understand the causes.
- What is an overdose and how do they happen? An overdose is when your body has more drugs in its system than it can handle. People can overdose on lots of things, including alcohol, cocaine/crack, opiates or a mixture of drugs. Opiate overdoses happen when the amount of opiates and/or other central nervous system depressants (downers) in your body causes your brain to shut down your breathing. If you can’t breathe, then you can’t get oxygen to your brain and after a little while your heart stops, which leads to death or permanent brain damage.
- As you know, there are a lot of things that can lead to overdosing on opiates. One important thing to consider is tolerance. This means the amount of drug that your body is used to and can handle. When you do opiates on a regular basis, your body begins to develop a tolerance to this and can handle more of the drug than someone who is not used to taking opiates regularly. A lot of people overdose when they use after taking a break for a while, and thus reduce their tolerance (because they were in drug treatment or jail for instance).
- Another factor that leads to opiate overdose is mixing opiates with other drugs, especially downers like Benzos (Valium Relanium, Seduxen, Clonopin) or Alcohol. When you combine downers you don’t just get an added effect, you get a multiplied effect. This means that when you combine these drugs the overall effect of ALL the drugs is increased. The more alcohol and/or downers you have in your system, the less heroin you will need to overdose.
- Physical state, that is the state your body is in, can also have an impact on the likelihood of overdose. If you are feeling sick or weak, your body may not be able to handle this usual amount of drugs that you are used to using.
- Another important thing to realize about opiates is that if you are buying them on the street you never really know how strong they are. A bag of heroin, for instance, can vary a lot in purity. If your body is used to dope that is only 10% heroin and you score really good stuff that’s 60% heroin, doing one bag of this is like doing 6 bags of the dope that your body is used to.

- Assess participant’s experience with overdose.
- What is your experience with overdose? If you experienced an overdose, why do you think it happened? What do you think is your current biggest risks for overdose? If you have not experienced overdose, why do you think that is? Have you witnessed an overdose? How did you respond?
- If you decide to inject drugs, here are some tips that may reduce the harm to you and maybe prevent an overdose.
- Know your tolerance. The more often you use opiates, and the greater the amounts you use, the higher your tolerance level, or the amount your body can handle. If you take a break from using for a few days or longer, your tolerance goes down drastically. This means that it will take less of the drug for you to get high when you use again. It also means that it will take less of the drug to cause an overdose. Therefore, if you take a break from using for a while, it’s important that you start out again slow; you can’t pick up where you left off.
- Know your supply. Because heroin is illegal, there is no way to know exactly how pure the heroin you get is. If you’re buying from a new source or getting a new batch of product, it’s important to test it out first to assess how good it is.
- Control Your Own High When someone else fixes your drugs for you or hits you off, you do not have complete control of what is going into your body. Try to fix your own drugs so you know exactly what’s going into the syringe. If you haven’t learned how to hit yourself, talk with a staff member of the Trust Point so they can give you some tips on how to inject yourself safely.
- Follow proper injection techniques, don’t slam the shot, especially if it is from a source you’re not used to or part of a new batch. Instead, after you register give several small pushes to “taste” the quality of the drug(s). Remember, once it’s in, you can’t get it out.
- Be aware of the risks of mixing drugs. Mixing heroin with other downers like alcohol, “benzos,” or prescription opiates can be especially dangerous. The drugs interact and can create a much more powerful effect than when they are used by themselves. If you are going to mix heroin with other downers, you may want to do the heroin first – especially if you are injecting because this gets the drug into your system very fast.
- Alcohol and pills come on more slowly and you may not get the full effects for a while after ingesting them. Also, alcohol and pills can interfere with your judgment and may result in you doing more heroin than you intended or not being as safe when using. The important thing is to be aware of what you’re taking and how different drugs can interact. Remember to pace yourself.
- Try not to use alone. If you are using alone and overdose, there is nobody there to call for help or to try and revive you. If you are going to use alone, it is especially important to follow the guidelines above, so you minimize the risk of overdosing. And if you find yourself along in an overdose situation and have called an ambulance, remember to unlock your door so that medical personnel can get inside your house.

- Introduce this section on recognizing the signs of overdose by drawing what the participant already knows.
- You may need to clarify any misinformation that is shared by using the following key points.
Recognizing the signs when someone is overdosing is critical in responding in enough time. Overdose rarely happens suddenly but most often comes on during a period of 1-3 hours. There are a number of signs that someone has overdosed on opiates. Can you name any of them?
Sometimes it may seem difficult to tell if someone is overdosing or they are just really high. Let’s review overdose signs with the following list:
- Passing out unconscious
- Awake but unable to talk
- Slow breathing (less than 12 breaths per minute)
- Choking or gurgling sounds
- Limp body
- Pale complexion
- Cold, clammy skin
- Turning blue (fingers and lips turn blue first)
- Vomiting
- Slow heartbeat/pulse
Let’s review difference using the following chart:
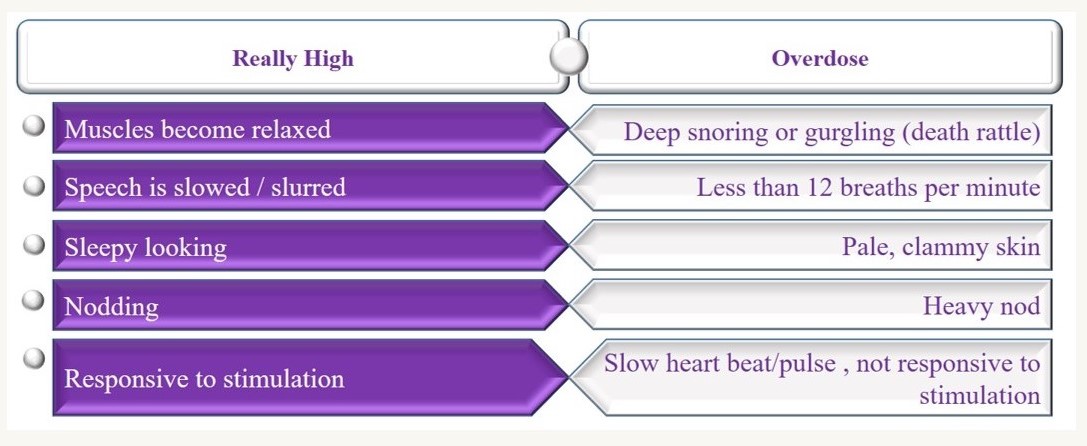
- If you are with someone who you think is overdosing, there are some steps that you can take to help them recover. There are also some strategies that people typically use which are not advised. Let us first go over what not to do:

- Don’t inject them with anything — it won’t work any more than physical stimulation and can waste time or make things worse depending on what you inject. An injection of salt water, for instance, could cause someone to go into cardiac arrest if they already have high sodium levels in their system. Injecting them with other drugs such as cocaine or speed may make the worse.
- Now let’s talk about what to do when someone is overdosing

Ask the participants to review the signs of an overdose:
- Deep snoring or gurgling (death rattle)
- Less than 12 breaths per minute
- Pale, clammy skin
- Heavy nod
- Slow heart beat/pulse, not responsive to stimulation
- After assessing the signs, if the person is unconscious or “out of it”, try to wake them up. Call their name and shake them. If this doesn’t work, try to wake them by causing mild pain like pinching them or rubbing your knuckles into their sternum, the place in the middle of your chest where your ribs meet (demonstrate and have the participant try rubbing knuckles in the middle of their chest).
- If this causes them to wake up, try to get them to focus. Can they speak to you? Try to get them to stand up and walk around, even if you have to support them. Check their breathing.
- If the person does not respond to stimulation and remains unconscious or their condition appears to get worse, follow these advise:
- Call for help (but don’t leave the person alone)
- Apply rescue breathing
- Administer Naloxone if trained to do so – if not trained, just break the ampoule and drop the solution to the victim’s mouth

- Ask participant what they have heard about Naloxone.
- Acknowledge correct responses and cover the following points about Naloxone:
- Naloxone is an injectable medication that reverses the effects of opiates like heroin. It is not a replacement for calling for emergency assistance but can save a life while getting help. We will give an introduction to when and how to use it in the next section.
- Regardless of your training, it is recommended that you call for an ambulance in the case of an overdose because it is important to have trained medical professionals assess the condition of the overdose victim. People who survive any type of overdose are at risk of experiencing other health complications as a result of the overdose, such as pneumonia and heart problems. Getting someone to be checked out by a medical professional is an important part of reducing the harms associated with overdosing.
- First, let’s talk about your thoughts regarding calling an ambulance in this situation. What are some of the reason why an ambulance may not be called during an overdose? You are right, some common responses you may hear are fear of police involvement, or delayed response, or stigma associated with drug users.
- When you call an ambulance, stay calm and ask those present to stay quiet. Have the address or location handy. If you don’t want to say it’s an overdose, tell the dispatcher that “the person has collapsed” and tell them whether or not they are breathing and whether or not they have a pulse.
- Focus on the symptoms rather than causes or diagnosis. Ambulance prioritizes cases of people who are not breathing, so if they aren‘t breathing or are barely breathing, make sure to emphasize that they aren‘t breathing.
- Ambulance personnel are more likely to contact police if the victim is found outside or in the entry way of a building. If victim is found in an apartment or a house, authorities are not contacted until the victim is taken to the hospital. Police is also contacted when there is a fatality or at the request of medical personnel. In these cases, police investigate if another person was responsible for the injection.
- If you have to leave the person at all, even for a minute to call ambulance, make sure you put them in the Recovery Position, which means laying the person slightly on their side, their body supported by a bent knee, with their face turned to the side.

- Refer to the Attika Foundation’s booklets during the conversation;
- Refer to Attika’ Foundations images of Recovery Position and explain that it can prevent the victim from choking on their own vomit if they begin to throw-up;
- Review steps in rescue breathing.
Download the Russian version of the booklet with overdose prevention guidelines applicable for situations when Naloxone is available:
Download the Russian version of the booklet with overdose prevention guidelines applicable for situations when Naloxone is not available:
- Now, we will talk about having access to and using Naloxone for an overdose of your family member, friend or someone you have witnessed in an overdose.
- Generally, Naloxone is an available medication used by doctors and nurses in emergency care for treatment of overdose, however, it has been shown to save more lives when available to injecting drug users and those that care about them. In Kyrgyzstan, Naloxone is available at NGOs who provide harm reduction services to those who use drugs. We will provide a list of locations for you today.
- Administering Naloxone does not require specific medical skills and can be provided by anyone who witnesses the opiate overdose, thus saving a great number of lives.
- Many countries around the world are currently using Naloxone to save lives. In the U.S. starting in 1999 it has been used to reverse the effects of opiate overdose while getting emergency care. Within three years of its use in non-medically administered programs deaths from overdose were reduced by between 30-42%.
- How does Naloxone work? Naloxone blocks the sedating and respiratory depressing effects of an opiate, like heroin. Naloxone replaces opiates on receptors and then blocks them for about 30-90 minutes causing sudden withdrawal. It does not get you high and has no addictive effects. You cannot overdose on Naloxone, and it has no effect if an opiate is not present.
- Naloxone is injected into a muscle and acts within 2-8 minutes, lasting 30-90 minutes. If no response is noticed with the first dose a second can be given with 2-5 minutes. Naloxone may also be available for nasal use at some sites.
- Naloxone should not be sold and should only be used with someone who is overdosing. There is no ability to get “high” from Naloxone and it will cause an immediate withdrawal for anyone using opioids.
- If you want, we will provide you with a supply Naloxone Kit with guidelines on when and how to administer Naloxone during an overdose.

- Ask participant if she has any concerns or foresees any barriers about using Naloxone.
- If the participant wants, give her Naloxone (make sure to pack the ampoules properly to prevent them from breaking), and help her to problem solve any barriers they identify that might prevent them from using the medicine.
- Summarize information about overdose.
- We provided you a lot of information about overdose today including what to do when someone else is overdosing. As we discussed, overdose does not have to be fatal. There are steps that you can take to prevent your own overdose, so if you do drugs, remember not to do them alone and do not use alcohol before injecting drugs.
- You will be safer if you inject first because it is easier to measure how much you drink than how much you inject. Lastly, if the steps to prevent overdose have not worked, we are very hopeful that through work with our collaborators we can offer this new option in preventing the death of your partner or those you care about.
- Before we move on, let’s brainstorm together and make a list of people in your community whom you could teach how to prevent overdose. Remember, we mentioned earlier that injecting drugs alone may be harmful to you. If you can teach these skills to someone in your community, you may be able to prevent your own overdose. I would also like to remind you to think of an individual(s) with whom you feel safe when doing drugs.

Through the link below you can download the short video with overdose prevention animated guidelines designed by Sergei Bessonov, the Executive Director for the National Harm Reduction Network Association — it is in 3gp format, “weighs” less than 8MB, so you can offer the participant to save it on their mobile phones and view when needed:
If you’d like to access the expanded version of the OD-prevention video guidelines designed and presented by Sergei Bessonov and his colleagues at Attika Foundation and the National Harm Reduction Network Association, and view it with the participant, just click the icon below and then save through the “save link as” command — it’s in MP4 format, the size it about 15MB:





















